COMMENT | The data shows that the Health Ministry is doing relatively well. The risk of a Covid-19 death per population in Malaysia is one per 50,000.
This compares favourably against the global average of one per 3,676.
It is worse in the UK and US, one per 700 and 781 respectively.
Singapore’s Covid-19 death per population is four times better at one per 200,000.
Put it another way, there are five, 20, 272, 1,280 and 1,429 deaths per million population in Singapore, Malaysia, World, US and UK respectively.
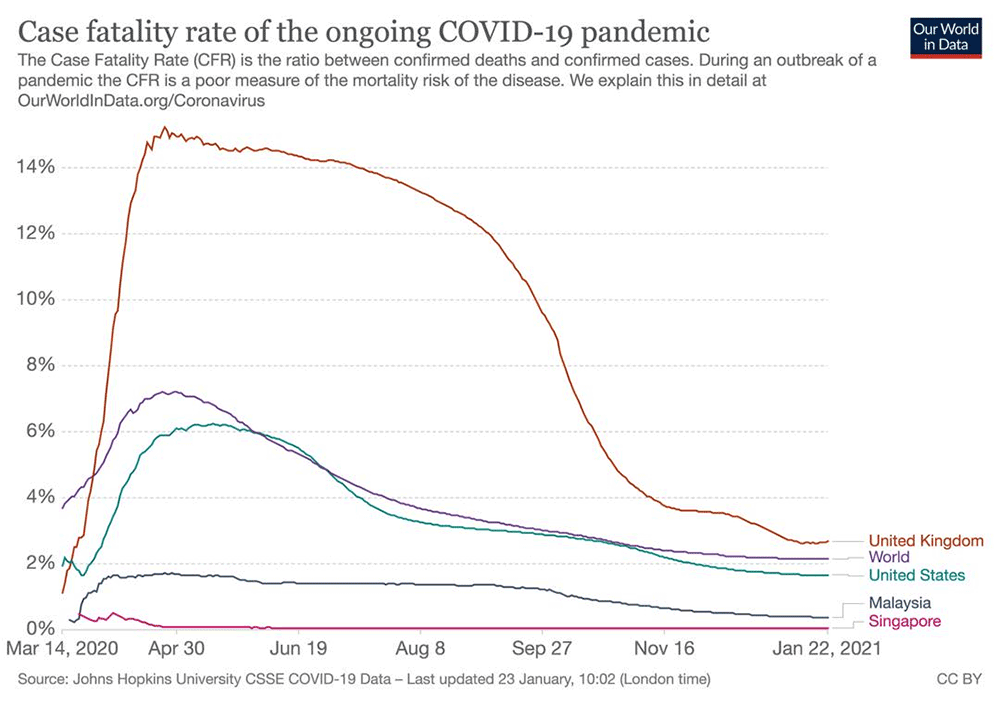
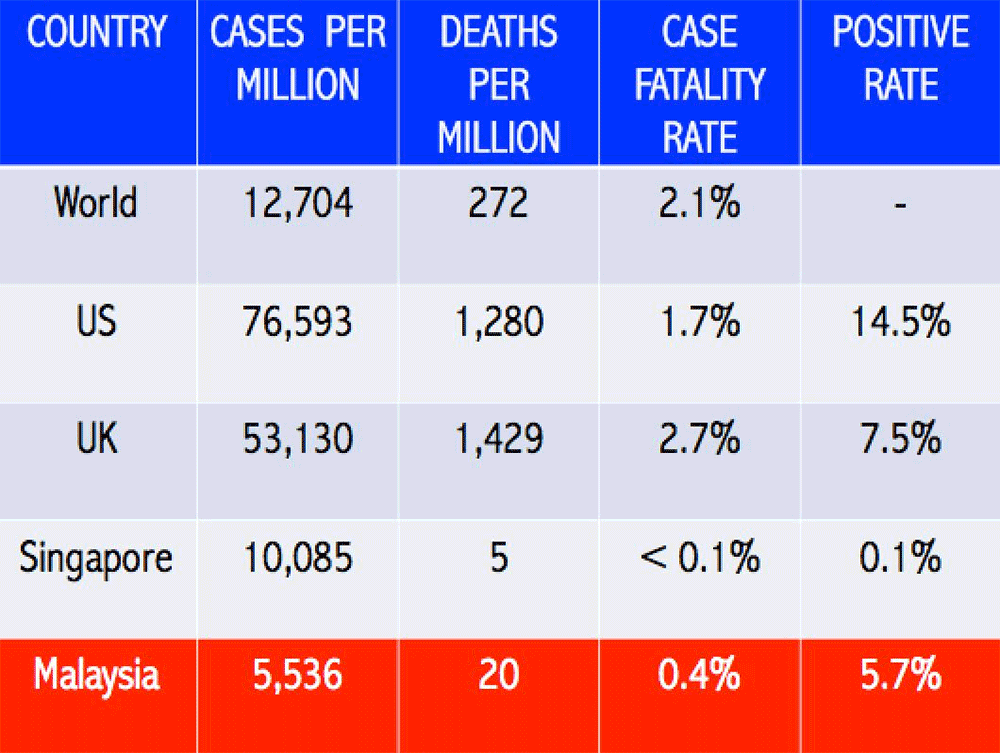
Testing and the consequent positive rate is a critical metric for understanding the pandemic, how it is spreading and whether it is under control or not. With this testing data, we can learn from the countries that are doing well at controlling the pandemic and which countries are just underreporting cases and deaths.
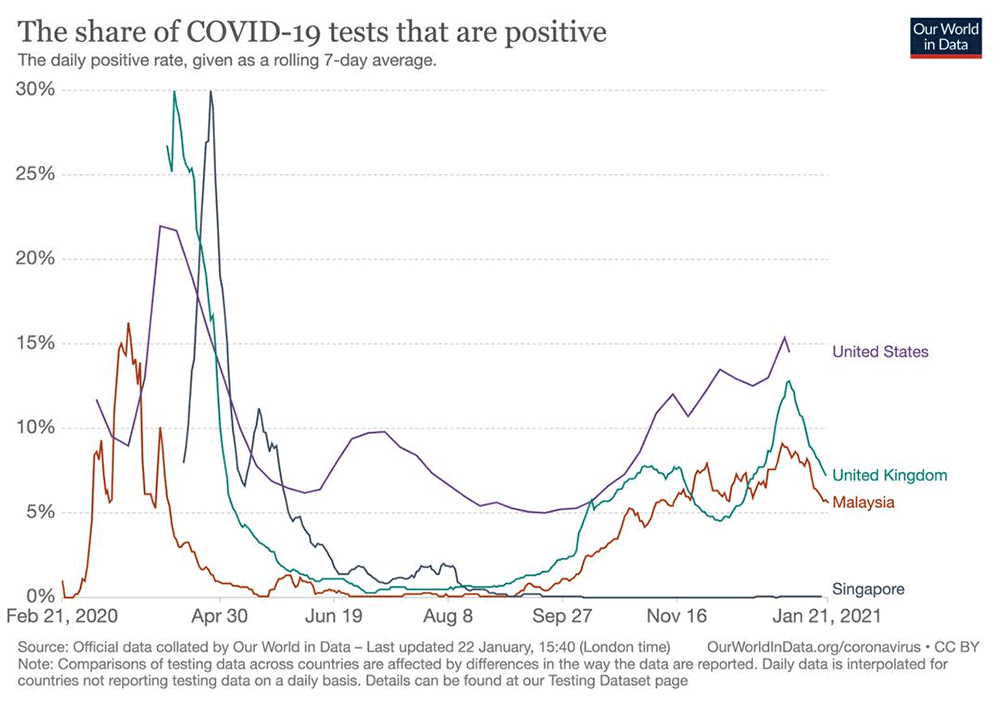
The most recent positive rate in the third quarter of January (seven-day rolling average) for Covid-19 testing is higher in the US and UK at 14.5 percent and 7.5 percent respectively, when compared to Malaysia at 5.7 percent and best in Singapore at less than 0.1 percent.
According to the World Health Organisation (WHO), a positive rate of more than 5 percent indicates that the epidemic is not quite under control in the country.
Prior to the onset of the third wave in Malayisa, the positive rate had dropped to less than 1 percent. This later rose to 9.1 percent in early January, and is now showing an encouraging downward trend. The countries doing best at pandemic control and mitigation have reported positive rates of less than 3 percent, which is a useful target to aim for.
Testing needs to be twinned with rapid isolation of cases and prompt tracing of contacts and their quarantine. This can only be achieved with a Rapid Test Kit-Antigen (RTK-Ag) with a turn-around time of less than 24 hours, made more affordable and can be undertaken at the point-of-care.
The PCR test which is presently utilised is not the best public health tool for Covid-19 surveillance purposes. It is best suited for analytical sensitivity and clinical diagnosis within the hospitals.
The fault tolerant time interval (FTTI) work process between the two testing regime looks like:
- RTK-Ag: Day 1 - test, Day 1 - results/isolate, Day 2 - trace/quarantine: Covid-19 busted
- PCR: Day 1 - test, Day 3 - result, Day 4 - inform, Day 5 to 7 - isolate/trace: Covid-19 spreads.
The integration of Covid-19 tracing apps MySejahtera with SeLangkah would be able to power an automated digital app, leveraging on data science and machine learning, to facilitate contact tracing and find hotspots in the country. This would mandate pre-emptive, targeted and mass screening as part of the FTTI rapid response to bust the Covid-19 clusters and mitigate the sporadic spread of the coronavirus.
Despite the surging numbers of Covid-19 cases, the Health Ministry infrastructure and services are holding up well and delivering good outcomes when compared to the US, UK and our southern neighbours. Therefore, if it ain’t broke, don’t fix it.
It is in this context that the following suggestions are made:
- The Health Ministry should continue to operate with the 52 dedicated Covid-19 hospitals.
- If these are inadequate to meet the current surge in Covid-19 cases, select private and government facilities can be transformed into dedicated Covid-19 hospitals.
- The concept and operations of hybrid hospitals should be avoided as much as possible. It compromises the quality of care, especially among Category 4-5 patients, and the safety of patients, healthcare workers, other hospital staff members and visitors, due to the real risk of nosocomial infection from this most transmissible coronavirus.
- The lay public is fast becoming very fearful of Covid-19 and hybrid hospitals and this has led to them shunning away from hospitals despite their need for regular visits and review.
- If they delay or miss their appointments, the management of non-Covid-19 illness such as non-communicable diseases, cancer, immunisation uptake, will be compromised.
- The Health Ministry has begun to decongest and create more empty general and Intensive Care Unit (ICU) beds in Covid-19 hospitals by discharging Category 1 and 2 patients to home isolation with clear instructions on the use of health assessment tools.
- The Health Ministry can also begin to start decanting non-Covid-19 patients in Covid-19 hospitals (occupying general/ICU/ventilator beds) to private hospitals to help accommodate Covid-19 patients.
- This smart triaging of cases will protect the capacity of our Covid-19 hospitals and allow private hospitals to play a bigger role in this private-public partnership in Covid-19 pandemic management.
DR MUSA MOHD NORDIN is a paediatrician and chairperson of the Federation of Islamic Medical Associations advisory council.
The views expressed here are those of the author/contributor and do not necessarily represent the views of Malaysiakini.

