LETTER | The recent polio case in Sabah highlights the people our health system has left behind. Therefore, we propose a Non-Citizens Health Act for Malaysia to achieve universal health coverage, which is both our health minister’s stated aim and a World Health Organisation commitment.
The Department of Statistics Malaysia estimates that there are 3.2 million non-citizens in 2019. Non-citizens is a broad term that encompass migrants (both legal and illegal, with another study estimating a total between 3.9 to 5.5 million people in Malaysia), refugees (estimated 180,000 people), and stateless people (at least 12,000 in West Malaysia and unknown numbers in Sabah comprising Bajau Laut, nomadic tribes, street children and children of migrant workers, and unwed foreigners with local partners).
Naturally, there are caveats. Calculations can differ for legitimate reasons, but it’s reasonable to believe that the official statistic undercounts the number of non-citizens. The list of categories is not exhaustive (e.g. foreign students and asylum-seekers aren’t included). Each category has different legal definitions, and the same individual might change categories over time. These are important caveats, but they can detract from more useful discussions about solutions.
Low or no access to health
The fundamental problem is easily articulated but difficult to solve. In general terms, Malaysia doesn’t even recognise the existence or concept of refugees, stateless people and illegal immigrants. As a result, non-citizens have almost no health rights and cannot meaningfully access Malaysia’s health system, either public or private.
Access to healthcare has many additional barriers: financial (too costly), legal (risk of arrest), physical (a nomadic lifestyle or life in remote jungle camps) or cultural (misinformation and fear). There are two insurance schemes for legal foreign workers, the Employment Injury Scheme by Socso or the Foreign Workers Hospitalisation and Surgical Insurance Scheme (Spika). However, the coverage is minimal, excludes outpatient treatment and maternal or antenatal care, and only supports legal workers.
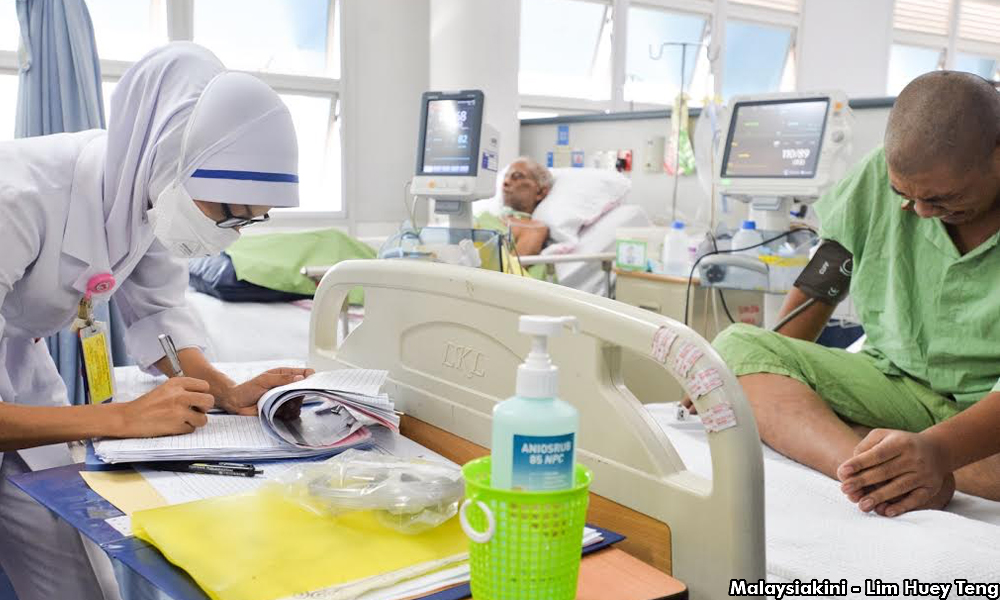
To make matters worse, non-citizens are charged between 24 to 100 times more than citizens to access care in public hospitals since January 2016, after the Fees Act (Medical) 1951 was amended for foreigners. The Immigration Act requires everyone to report the presence of undocumented foreigners to the police, which creates an ethical dilemma for doctors and nurses simply trying to save a life. Private care is generally unaffordable to non-citizens other than very basic care at general practitioner clinics. Private hospitalisation is almost completely inaccessible, except for ad hoc interventions by private hospitals and non-governmental organisations.
Reasons to extend health rights
There are many reasons to extend health rights to non-citizens, especially children and pregnant women. Many are powerful moral, ethical, humanistic, religious, philosophical, international law and human rights reasons. There is also the public health case, especially if we want to prevent communicable diseases among citizens and non-citizens alike. There is even an economic case to provide health rights to migrants, because healthier migrants will increase Malaysia’s prosperity.
However, we are aware of countervailing political realities. The justice of utilising scarce taxpayer ringgit for non-taxpayers is an important consideration. Malaysia has to secure our borders because our generosity can’t be bottomless. There could be pushback from Malaysians whose own rights are still being secured, and Malaysia could be a more attractive destination for free riders.
Proposing a framework
After carefully considering both the case for and against providing health rights to non-citizens, we believe that Malaysia must pass a Non-Citizens Health Act to provide certain health rights for non-citizens. In this letter, we propose a realistic framework for action.
This Act will prescribe basic health rights for all non-citizens, starting with vaccinations, maternal and antenatal care, child health up to the age of five and treatment for certain communicable diseases such as pulmonary tuberculosis. Maternal health should include sensitive, non-coercive and thoughtfully delivered family planning services so that non-citizens do not misperceive this as attempting to control their numbers. The government can consider additional services at regular intervals of three to five years, because international standards, health systems and financing capabilities would evolve over time.
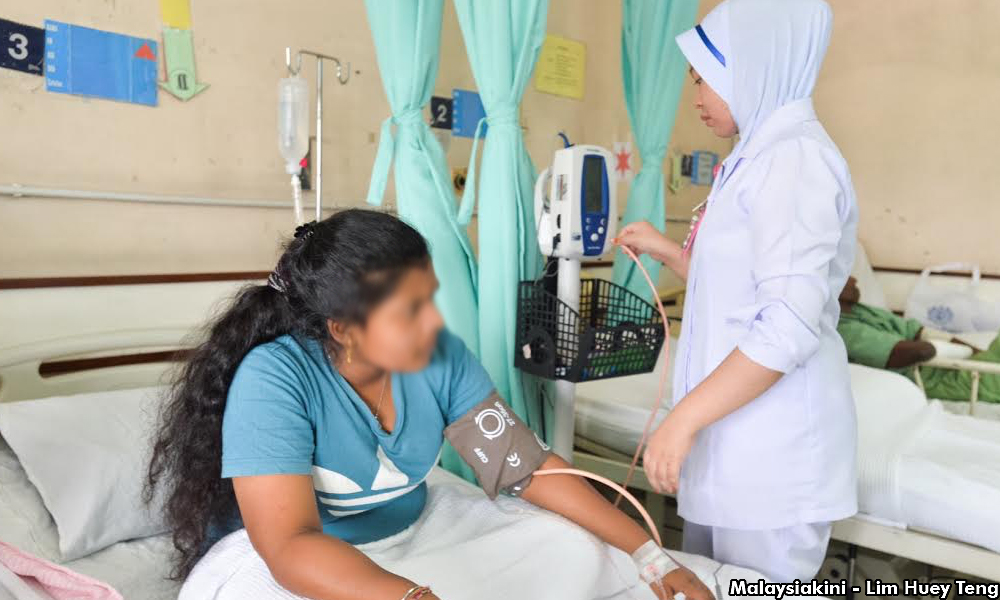
These services must be provided free or nearly free, alongside effective education and decriminalising non-citizens’ attendance in public health facilities. The funds can come from a combination of existing levies on foreign workers, private insurance or taxation. All non-citizens should be allowed (indeed, encouraged) to purchase private insurance similar to Thailand since 2001, and this can be run by NGOs on a privately-held, non-profit basis. Allowing more non-citizens, legal or otherwise, to purchase health insurance reduces adverse selection, increases the risk-pooling effect and may even reduce the premiums over time.
The public health reason for enshrining such rights deserve an elaboration. Thailand has kept its rates of tuberculosis at a constant low, despite the influx of migrants from Myanmar and Indochina with higher rates of tuberculosis. This is due to their dual policy of extending health rights to all migrants while simultaneously securing their borders. If Malaysia continues to pretend that non-citizens don’t exist within our borders, we’ll see more outbreaks of polio and tuberculosis on top of the human cost of the unnecessary disease.
There are also compelling ethical and logical reasons to enshrine these rights. Children and mothers are among the most vulnerable populations, and they deserve our care. Preventive care is cheap and cost-effective. It will not only avoid outbreaks but also emergencies when non-citizens come to hospitals with massive complications requiring heroic (and expensive) curative care.
The standard practice on the ground is to provide emergency life-saving measures for foreigners, although this is not explicitly mandated, allowed or prohibited by the government. In this silence, doctors and nurses will do what they deem necessary for the patient’s benefit. Therefore, the Act must protect healthcare professionals from punitive action if non-citizens fail to settle hospital bills. This Act must also remove the requirement for health professionals to inform the Immigration Department if they are treating undocumented migrants, to avoid a professional conflict of interest.
Enshrining this Act is not enough. The Malaysian government must also implement durable legal solutions for all categories of non-citizens in Malaysia. In addition, the national registration pathways must be strengthened so that every child born in the interior parts of Malaysia will receive the MyKad, which determines their legal rights as Malaysians, including health and education. The crucial point is that debates and decisions must take place, instead of Malaysia negligently sitting on a time-bomb.
We urge the government to debate and then pass the Non-Citizens Health Act, and assert our soft power by demonstrating a humane, practical and politically feasible solution to the world.
This letter is signed by:
Dr Khor Swee Kheng
Dr John Teo
Professor Pang Yong Kek (President, Malaysian Thoracic Society)
Professor Tang Swee Fong (Secretary, Malaysian Pediatrics Association)
Federation of Reproductive Health Associations, Malaysia (FRHAM)
Heidy Quah (President, Refuge for the Refugees)
James Bawi Thang Bik (President, Alliance of Chin Refugees)
All Women’s Action Society (Awam)
Dr Amar Singh-HSS
Dr Subatra Jayaraj
Dr Ravindran Jegasothy
Dr Timothy Cheng
The views expressed here are those of the author/contributor and do not necessarily represent the views of Malaysiakini.

