COMMENT | I’d like to address three recent issues in our health system. They may seem easy to solve with our usual short-term solutions, but in reality, they mask much larger and deeper problems that need difficult and long-term structural reforms.
In December 2019, the government announced a surprise decision to stop regulating the consultation fees of private-sector doctors. This leaves the procedure fees of doctors as the only remaining cost category that is regulated. It’s only a matter of time before even this category is removed, with the task of controlling healthcare prices being left to market forces, i.e. consumers.
Markets are a reasonable ideological, political and economic stance and they are very successful in many other sectors. However, market failures in the healthcare sector are plentiful. Therefore, exceedingly few countries leave healthcare cost control entirely to the market and consumers. The biggest (and scariest) example is the US which spends US$3.5 trillion a year on healthcare without getting world-leading results.

The Malaysian government can deregulate every cost category in the long-term and it can be a reasonable policy position. However, they must simultaneously correct for market failures. The ministry must implement solutions to improve price transparency to consumers (by private hospitals, drug companies, individual doctors and other stakeholders), publish fee benchmarks (e.g. Singapore’s Health Ministry publishes the price structures of private surgeons) and aggressively fight cartels and unfair prices (by empowering the Malaysian Competition Commission and consumer associations).
None of these is yet in the "Sihat Bersama 2030" (SB2030) plan. That plan also does not address the philosophical role of private sector healthcare in Malaysia, including questions like “should we profit from healthcare” and the role of government-linked corporations (GLCs) who own private hospitals.
There’s a political need to control prices in the private sector. High prices will drive consumers to the already-overstretched public sector, which will lead to longer queues, poorer service and worse outcomes. That can lead to any government losing legitimacy and elections, when the social contract of “free healthcare services for votes” is broken.
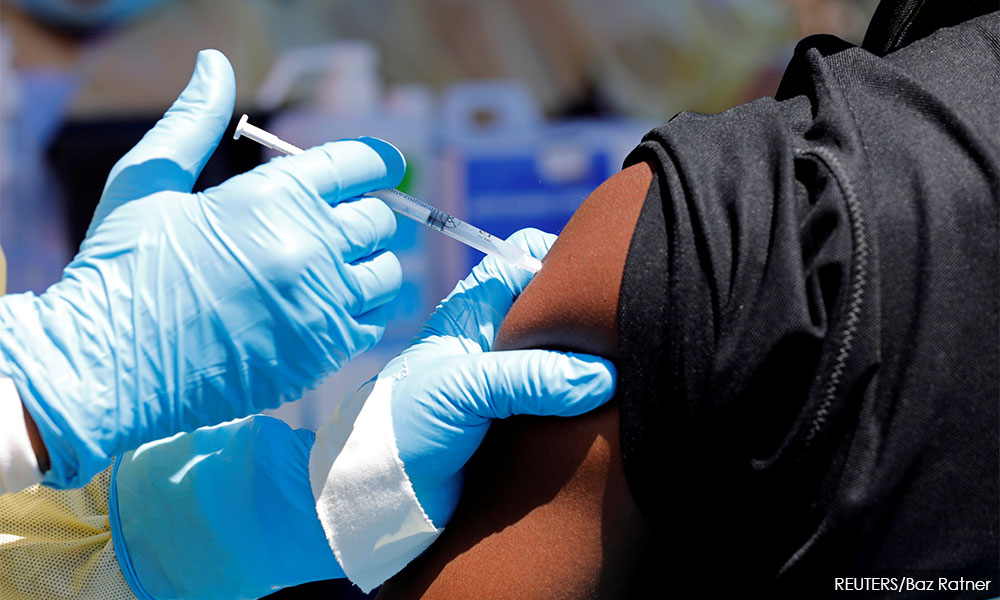
Our Health Ministry is taking robust and correct measures to address the current polio outbreak in Sabah, and kudos to them. It is admirable that we are collaborating with WHO, Unicef and the Philippines government, and timely that this crisis has woken up Malaysia to the importance of vaccinations.
However well we manage this outbreak today, there will be more on the way. I’ve previously written about the importance of migrant health and the domestic politics and international geopolitics of the polio outbreak in Sabah, describing how the health of migrants is a time bomb that we have sat on for too long.
This outbreak can and should force the SB2030 plan to consider the health of non-citizens in Malaysia in ways that are balanced and appropriate in political, border security and geopolitical terms. In simple terms, provide non-citizens with certain limited health rights and pay for it through a combination of our taxes and their insurance premiums.
Since 2001, Thailand has allowed non-citizens to purchase health insurance and simultaneously apply for work permits as part of its efforts to manage undocumented migrants. That can be a model Malaysia can modify and adapt for ourselves.
We can no longer pretend that refugees and illegal migrants do not exist in Malaysia, or allow alleged citizenship-for-votes scandals to ruin our reputation. The Sabah Temporary Pass (PSS) debate is a healthy and overdue one, because it’s taking place in the public domain and away from the shadows. We need more such debates today, to build durable solutions for our health system tomorrow.
In that same December week, the government decided to abolish the critical services allowance and then decided to postpone that decision after a public outcry. That allowance is one of many granted under the "Skim Saraan Malaysia" that was launched in 2002 but has not been revised since.
In my opinion, the allowances are helpful to attract and retain (health) professionals in the public sector and are a good alternative to raising salaries. They can be flexibly introduced or withdrawn and have little impact on pensions commitments, allowing the government to be fiscally responsible.

Although the critical service allowance has been reinstated, the complex problems won’t end there. Firstly, the public healthcare service is underpaid, leading to a brain drain to the private sector and internationally. Secondly, we must resolve the dilemma of trimming down a bloated civil service while bolstering up an understaffed health service. Thirdly, the Public Service Department (PSD) must share “hiring, remunerating, promoting and firing” privileges with the Health Ministry.
The SB2030 plan also lists corporatisation as a pillar to resolve financing and human capital challenges. This could be a move in the right direction if done correctly. Corporatisation is not privatisation, and hospitals will not be turned into profit-making entities. Hospitals can be privately-owned non-profit entities held by voluntary organisations or even the government.
For example, 80 percent of hospitals in Japan are privately-owned non-profit hospitals, just like many hospitals in Canada and even the foundation trusts in the National Health System in the UK.

The crucial theme in corporatisation is not ownership but governance and operations. The Malaysian government can continue owning the assets (building, land, MRI machines) indirectly, but oversight, operations, strategy and human resources aspects are left to the individual entities.
This removes an existing conflict of interest where the Health Ministry is simultaneously a payer, provider, regulator and asset owner. The ministry can then focus on being a payer and regulator, allowing the newly created corporate non-profit bodies to become the provider and asset-owner.
Allowing hospitals or cluster hospitals to be corporatised could be an elegant long-term solution to problems of chronic low pay, the dilemma between downsizing the civil service and upsizing the health service and the co-sharing of human resources decisions between the ministry and the PSD.
SB2030 must address these deeper fundamental problems, instead of focusing only on superficial and populist short-term solutions.
SWEE KHENG KHOR is now at the Blavatnik School of Government at Oxford. He holds an MD (Universiti Kebangsaan Malaysia), an MPH (University of California, Berkeley) and membership of the Royal College of Physicians, UK.
The views expressed here are those of the author/contributor and do not necessarily represent the views of Malaysiakini.

